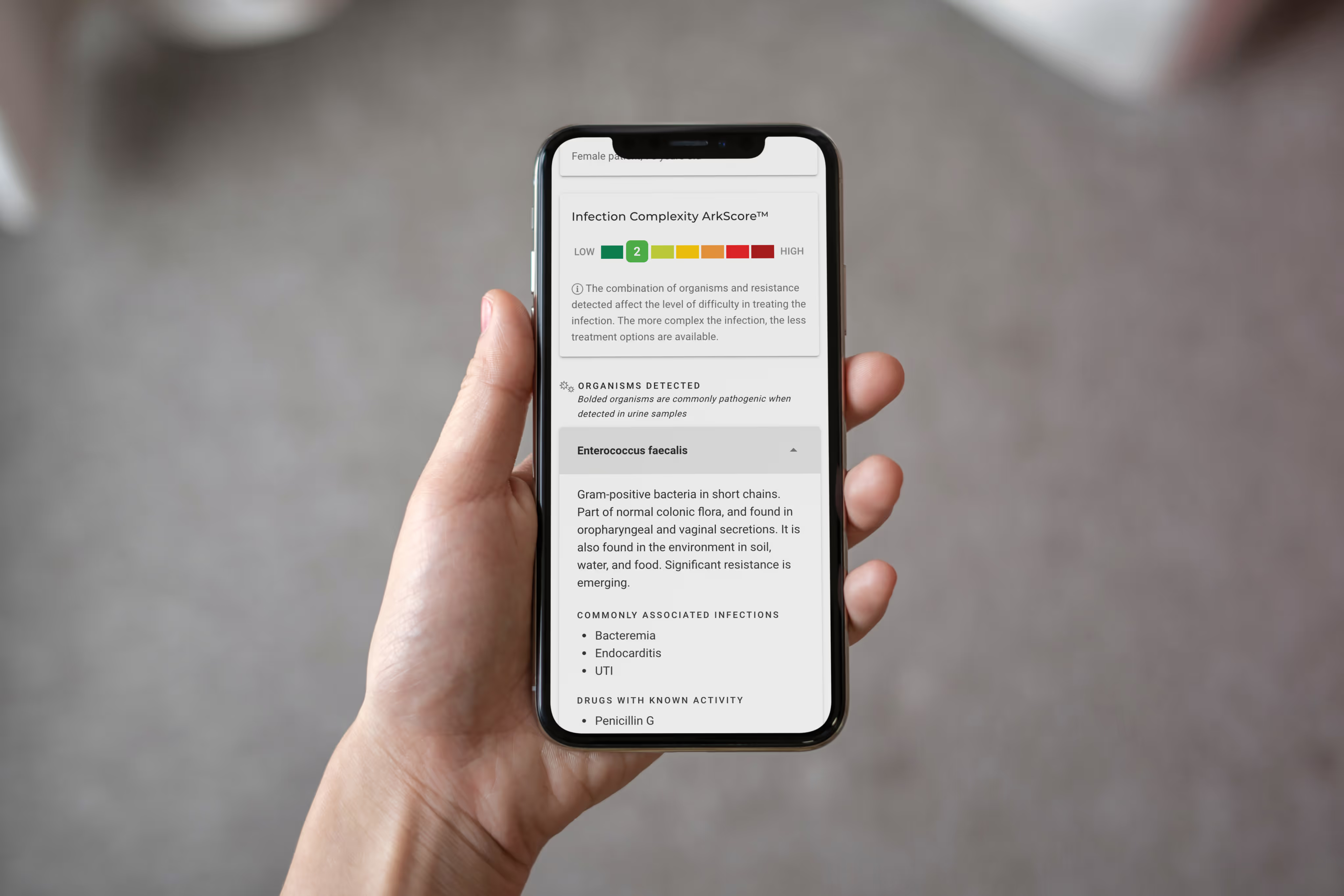
How Arkstone saves healthcare payers billions by eliminating unnecessary prescriptions
Most patients never know how often the right antibiotic is a guess. A faster, more confident answer changes everything for the patient, the clinician, and the hospital.
Arkstone's platform drives cost savings by enabling earlier, more accurate treatment decisions. Clinicians initiate targeted therapy sooner, leading to shorter hospital stays, fewer complications, and reduced use of broad-spectrum antibiotics. Rigorous validation and a human-in-the-loop approach minimize treatment errors and rework, while improved stewardship lowers pharmacy costs and helps prevent expensive resistance-related cases. The result: meaningful savings at both the patient level (fewer adverse events, faster recovery) and the system level (lower length of stay, optimized resource utilization).
Antibiotics are one of the most powerful tools in modern medicine. They are also one of the most overused. In 2022 alone, clinicians in the United States wrote 236 million outpatient antibiotic prescriptions, roughly 709 prescriptions for every 1,000 Americans. Antibiotics are prescribed for everything from sore throats to sinus infections to ear pain. The CDC estimates that 30% or more of those prescriptions are unnecessary, and many more could be improved through better antibiotic choice, dosing, or duration.
The consequences are enormous.
Inappropriate antibiotic prescribing adds an estimated $3.4 billion in excess healthcare costs every year. Antibiotic-resistant infections add more than $2 billion in direct costs, and just six major resistant pathogens alone cost the U.S. healthcare system over $4.6 billion annually.
But behind those numbers is a simple reality: most antibiotic decisions are made quickly, often with limited information, under significant time pressure. Clinicians want to do the right thing, but the healthcare system rarely gives them the tools to make optimal antimicrobial decisions in the moment.
That’s the problem Arkstone set out to solve.
To date, Arkstone has delivered approximately 1.5 million antibiotic decision interventions, moments where clinicians used Arkstone’s guidance to determine whether an antibiotic was necessary and, if so, which antibiotic, dose, and duration was most appropriate.
Across these interventions, Arkstone determined that antibiotics were unnecessary in up to 70% of cases for certain infection types. When treatment was recommended, Arkstone often suggested lower-cost antibiotic options, shorter courses of therapy, and optimized dosing consistent with antimicrobial stewardship best practices.
Even with conservative assumptions, the impact is already measurable. If we assume an average outpatient antibiotic costs $15–$25 per course, Arkstone has likely prevented between 450,000 and 1,050,000 unnecessary prescriptions. That alone translates to roughly $8 million to $37 million in avoided antibiotic spending.
And that estimate only captures the pharmacy cost of the drug itself. It does not include the downstream costs of adverse drug reactions, unnecessary follow-up visits, Clostridioides difficile infections, or the growing burden of antimicrobial resistance — all of which multiply the true cost of inappropriate prescribing.
But the more important story is not what Arkstone has already done.
It’s what happens when this kind of intervention scales.
Those 1.5 million interventions represent the equivalent of about 0.6% of all outpatient antibiotic prescriptions written in the United States in a single year. In other words, Arkstone has already influenced a meaningful slice of antibiotic decision-making — but only a tiny fraction of the total system.
Now imagine something different.
Today, antibiotic stewardship largely happens after the prescription has already been written. Hospitals run retrospective reviews. Pharmacists monitor trends. Committees publish guidelines. But the decision — the moment when a patient either receives an antibiotic or doesn’t — has already passed.
What if stewardship happened before the antibiotic was dispensed?
Imagine a world where every antibiotic prescription passed through a real-time clinical intelligence layer — something that could instantly evaluate symptoms, diagnoses, patient risk factors, guideline recommendations, and local resistance patterns before the medication ever reached the pharmacy counter.
If the antibiotic were appropriate, the prescription would proceed immediately.
If it weren’t, the prescriber would receive an immediate recommendation: no antibiotic, a different agent, a lower dose, or a shorter course.
This is not a radical idea. Healthcare already does this for expensive drugs through prior authorization systems. Yet antibiotics — one of the most overused and systemically harmful drug classes in medicine — rarely undergo any real-time review.
The scale of impact would be extraordinary.
If Arkstone intervened across all outpatient antibiotic prescribing in the United States, and prevented just 30% of prescriptions, that would eliminate roughly 71 million unnecessary antibiotic courses every year. At average drug costs, that alone represents $1.1 to $1.8 billion in annual pharmacy savings.
But the real impact would be far larger: fewer adverse drug reactions, fewer secondary infections, fewer resistant organisms, and fewer hospitalizations tied to inappropriate antimicrobial use.
Consider what this could look like inside a single healthcare system.
The Veterans Health Administration serves roughly 9 million patients. Based on national prescribing rates, that population likely receives about 6.4 million outpatient antibiotics each year. If Arkstone prevented 30% of unnecessary prescriptions, that would mean nearly 2 million antibiotics avoided annually — representing roughly $30 to $50 million in direct pharmacy savings every year, before accounting for downstream clinical benefits.
Multiply that across large integrated health systems, outpatient networks, and retail pharmacy chains, and the scale becomes clear. Antibiotic resistance is often described as one of the defining public health threats of the century. Yet unlike many healthcare crises, the solution here is not a new drug, a new vaccine, or a breakthrough therapy.
The solution is better decisions at the moment antibiotics are prescribed. Arkstone is already proving that those decisions can be improved. With 1.5 million antibiotic interventions, the company has demonstrated that targeted, real-time guidance can meaningfully reduce unnecessary antibiotic use while steering clinicians toward safer and more cost-effective treatments.
But that number — 1.5 million — is still just the beginning. Because if we can influence 1.5 million antibiotic decisions, we can influence 15 million. And if we can influence 15 million, we can influence 150 million. The question is no longer whether better antibiotic stewardship is possible. The question is how quickly we can scale it. And perhaps more importantly, who is willing to lead that change.
Solving antibiotic misuse at scale will not happen through technology alone. It will require health systems, pharmacies, payers, and government partners willing to rethink how antibiotics are prescribed, dispensed, and monitored. The tools to dramatically reduce inappropriate antibiotic use already exist.
The real question is:
Who is ready to partner with Arkstone to address this challenge?
Share this article
Blogs
Latest Blogs
Stay informed with our featured blogs.

When Negative Cultures Lie: The Hidden Cost of Diagnostic Blind Spots
When a culture comes back negative, most clinicians take it at face value. But a negative result is only as reliable as the method used to obtain it.
When a culture comes back negative, most clinicians take it at face value. But a negative result is only as reliable as the method used to obtain it.

When Antibiotics Miss the Mark Prescribe Responsibly · Episode 2
A conversation with Tami Burdick, Patient Advocate and Author of Diagnosis Detective: Curing Granulomatous Mastitis.
A conversation with Tami Burdick, Patient Advocate and Author of Diagnosis Detective: Curing Granulomatous Mastitis.

How Arkstone saves healthcare payers billions by eliminating unnecessary prescriptions
Most patients never know how often the right antibiotic is a guess. A faster, more confident answer changes everything for the patient, the clinician, and the hospital.
Most patients never know how often the right antibiotic is a guess. A faster, more confident answer changes everything for the patient, the clinician, and the hospital.
Customer Testimonials
Arkstone's solutions have transformed our patient care.
Take the Next Step, Try OneChoice®
No more guesswork. No more lookup tools. No more inaccuracies and inconsistencies. No more stopping to ask for directions.